Showing posts with label CARDIOLOGY. Show all posts
Showing posts with label CARDIOLOGY. Show all posts
Tuesday, 9 August 2011
Friday, 22 July 2011
Papillary muscle Rupture
Rupture of a papillary muscle is usually associated with an infarction of which area of myocardium?
Diagnosis of papillary muscle dysfunction or rupture may be made on echocardiography or by measuring large V waves in the pulmonary artery wedge pressure with a Swan-Ganz catheter.
- (A) Inferior
- (B) Inferior–posterior
- (C) Lateral
- (D) Anterior
- (E) Anteroseptal
The answer is B.
Papillary muscle rupture is usually associated with an inferior–posterior infarction and involves the posterior papillary muscle. Outcome depends on whether the entire muscle body or only the head is ruptured. Rupture of an entire muscle body is associated with a high mortality rate (up to 50 percent within 24 h).Diagnosis of papillary muscle dysfunction or rupture may be made on echocardiography or by measuring large V waves in the pulmonary artery wedge pressure with a Swan-Ganz catheter.
Papillary Muscle Infarct with Rupture: Gross, an excellent example of ruptured papillary muscle.
Wednesday, 25 May 2011
Causes, Symptoms and sings of aortic valvular insufficiency
A 74-year-old man presents with exertional dyspnea and generalized weakness. On examination, you discover a high-pitched, blowing diastolic murmur and a wide pulse pressure with bounding pulses. The most likely diagnosis is?
- A) aortic stenosis
- B) aortic insufficiency
- C) mitral stenosis
- D) mitral insufficiency
- E) coarctation of the aorta
Answer and Discussion
The answer is B.Causes of aortic regurgitation :
The prevalence of aortic regurgitation increases with age. Unlike aortic valve stenosis, aortic valvular insufficiency is rarely caused by degenerative aortic valve disease. Acute aortic valvular insufficiency may be due to infective endocarditis, aortic dissection, trauma, or rupture of the sinus of Valsalva. Chronic aortic insufficiency can be caused by valve leaflet disease, including rheumatic heart disease, congenital heart disease, rheumatoid arthritis, ankylosing spondylitis, or myxomatous degeneration. Chronic aortic insufficiency may also be caused by aortic root disease secondary to systemic hypertension, syphilitic aortitis, cystic medial necrosis, ankylosing spondylitis, rheumatoid arthritis, Reiter's disease, systemic lupus erythematosus, Ehlers–Danlos syndrome, and pseudoxanthoma elasticum.Symptoms and sings of aortic valvular insufficiency :
The symptoms of aortic valvular insufficiency are the same in older persons as they are in younger ones. Usually, the main symptoms are related to heart failure, with exertional dyspnea and weakness being common symptoms. In some elderly patients, symptoms of dyspnea and palpitations may be more common at rest than with exertion. Nocturnal angina pectoris, often accompanied by flushing, diaphoresis, and palpitations, may occur; this is thought to be related to the slowing of the heart rate and the drop of arterial diastolic pressure. The classic findings of a high-pitched, blowing diastolic murmur and a wide pulse pressure with an abruptly rising and collapsing pulse should make the diagnosis of aortic valvular insufficiency easily recognized in elderly patients.
Saturday, 14 May 2011
Triad of Kartagener syndrome
A 14-year-old boy presents with a history of chronic sinusitis and frequent pneumonias. On physical examination, the patient has normal vital signs and is afebrile. He has mild frontal and maxillary sinus tenderness with palpation. Transillumination of the sinuses is normal. Heart sounds are best heard on the right side of the chest. The boy is coughing copious amounts of yellowish sputum. Which of the following is the most likely diagnosis?
The answer is b."Kartagener syndrome"
Kartagener syndrome is the inheritable disorder of dextrocardia, chronic sinusitis (with the formation of nasal polyps), and bronchiectasis. Patients may also present with situs inversus.The disorder is due to a defect that causes the cilia within the respiratory tract epithelium to become immotile. Cilia of the sperm are also affected.
- a.Cystic fibrosis
- b.Kartagener syndrome
- c.Pulmonary dysplasia
- d.Tuberculosis
- e.Pulmonary hypertension
The answer is b."Kartagener syndrome"
Kartagener syndrome is the inheritable disorder of dextrocardia, chronic sinusitis (with the formation of nasal polyps), and bronchiectasis. Patients may also present with situs inversus.The disorder is due to a defect that causes the cilia within the respiratory tract epithelium to become immotile. Cilia of the sperm are also affected.
Frontal and Chest x-ray showing dextrocardia "the typical radiographic sign of Kartagener's syndrom" and bronchiectasis.
Wednesday, 6 April 2011
Images for Skin manifestations in hyperlipidemia
Xanthelasma in a 43-year-old patient with hyper-cholesterolemia.
-Severe hyperlipidemia, particularly primary forms of hyperlipidemia, can be associated with lipid deposits in the skin and in joints. However, a corneal arcus, an arcus lipoides, and xanthelasma may be present with normal cholesterol levels after the age of 40.
-Tendon xanthoma and palmar xanthoma occur in some of the primary dyslipoproteinemias.
Tendinous xanthomas are nodose, subcutaneous lesions attached to ligaments and tendons, particularly the Achilles tendon due to accumulations of lipid-laden macrophages (foam cells) in tendons.
The nodules may be yellowish, but are usually skin colored. They are often associated with other xanthomas, and indicate the presence of hypercholesterolemia or other lipid abnormality.
-Also Tubero-eruptive xanthoma that may itch and the lesions may be reddened due to inflammation and scratch effects.
Eruptive xanthoma in hyperlipidemia.
Monday, 4 April 2011
Gross pathology of Atherosclerosis in Aorta
Atherosclerosis is the process in which deposits of fatty substances, cholesterol, cellular waste products, calcium and other substances build up in the inner lining of an artery "Plaque".
Clinical Consequences of Atheromatous plaques include:
* Occlusion
* Vessel rupture
* Aneurysmal dissection
Distribution of atheromatous plaques:
- Lower descending aorta {ostia of the major branches}
- First 3 inches of coronary arteries
- Descending aorta
- Internal carotids
- Circle of Willis
- Leg arteries
Clinical Consequences of Atheromatous plaques include:
* Occlusion
* Vessel rupture
* Aneurysmal dissection
Tuesday, 15 March 2011
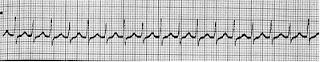
ECG of Supraventricular tachycardia
A 36-year-old white female nurse comes to the ER due to a sensation of fast heart rate, slight dizziness, and vague chest fullness. Blood pressure is 110/70. The following rhythm strip is obtained, which shows which of the following?
Atrial fibrillation would show an irregularly irregular rhythm without discrete P waves. Wide QRS complexes with rate greater than 100 would be expected in ventricular tachycardia.
- a.Atrial fibrillation
- b.Atrial flutter
- c.Supraventricular tachycardia
- d.Ventricular tachycardia
The answer is (c).
Paroxysmal supraventricular tachycardia due to AV nodal reentry typically displays a narrow QRS complex without clearly discernible P waves, with a rate in the 160 to 190 range. The atrial rate is faster in atrial flutter, typically with a classic sawtooth pattern of P waves, with AV conduction ratios most commonly 2:1 or 4:1, leading to ventricular rates of 150 or 75 per min. Atrial fibrillation would show an irregularly irregular rhythm without discrete P waves. Wide QRS complexes with rate greater than 100 would be expected in ventricular tachycardia.
Thursday, 27 January 2011
ECG changes in acute MI
The ECG changes are often critical in the diagnosis of acute MI and guiding therapy.
There is a series of ECG changes reflect the evolution of the infarction (The Figure below).
1.The earliest changes are : tall, positive, hyper acute T waves in the ischemic vascular territory.
2.This is followed by elevation of the ST segments (myocardial “injury pattern”).
3.Over hours to days, T-wave inversion frequently develops.
4.And finally, diminished R-wave amplitude or Q waves occur, representing significant myocardial necrosis and replacement by scar tissue, and they are what one seeks to prevent in treating the acute MI .
There is a series of ECG changes reflect the evolution of the infarction (The Figure below).
1.The earliest changes are : tall, positive, hyper acute T waves in the ischemic vascular territory.
2.This is followed by elevation of the ST segments (myocardial “injury pattern”).
3.Over hours to days, T-wave inversion frequently develops.
4.And finally, diminished R-wave amplitude or Q waves occur, representing significant myocardial necrosis and replacement by scar tissue, and they are what one seeks to prevent in treating the acute MI .
Temporal evolution of ECG changes in acute myocardial infarction.
Note the tall hyperacute T waves and loss of R-wave amplitude,followed by ST-segment elevation,T-wave inversion,and development of Q waves.Persistent ST-segment elevation suggests left ventricular aneurysm.
Thursday, 6 January 2011
Types of Coarctation of the aorta
Infantile type :- aortic stenosis proximal to insertion of ductus arteriosus (preductal).
Adult type :- stenosis is distal to ductus arteriosus (postductal). Associated with notching of the ribs (due to collateral circulation), hypertension in upper extremities, weak pulses in lower extremities,
Associated wilh Turner's syndrome.
Can result in aortic regurgitation.
Check femoral pulses on physical exam.
ADult: Distal to Ductus. Most commonly associated with bicuspid aortic valve.
Adult type :- stenosis is distal to ductus arteriosus (postductal). Associated with notching of the ribs (due to collateral circulation), hypertension in upper extremities, weak pulses in lower extremities,
Associated wilh Turner's syndrome.
Can result in aortic regurgitation.
Check femoral pulses on physical exam.
SO ;
INfantile: IN close to the heart. ADult: Distal to Ductus. Most commonly associated with bicuspid aortic valve.
Wednesday, 5 January 2011
Different arterial pulse waveforms and example causes
This is best assessed at the carotid artery. You are feeling for the speed at which the artery expands and collapses and force with which it does so. It takes some practise to master and it may be useful to imagine a graph such as those shown in the figure below,also Some examples are present:
Aortic stenosis: a slow rising pulse, maybe with a palpable shudder. Sometimes called anacrotic or a plateau phase.
Aortic regurgitation: a collapsing pulse which feels as though it suddenly hits your fingers and falls away just as quickly. You could try feeling at the brachial artery and raising the arm above the patient's heart. Sometimes referred to as a waterhammer pulse.
Pulsus bisferiens: a waveform with 2 peaks, found where aortic stenosis and regurgitation co-exist.
Hypertrophic cardiomyopathy: this pulse may feel normal at first but peter out quickly. Often described as jerky.
Pulsus alternans: an alternating strong and weak pulsation, synonymous with a severely impaired left ventricle in a failing heart.
Pulsus paradoxus: pulse is weaker during inspiration (causes include cardiac tamponade, status asthmaticus, and constrictive pericarditis).
Aortic stenosis: a slow rising pulse, maybe with a palpable shudder. Sometimes called anacrotic or a plateau phase.
Aortic regurgitation: a collapsing pulse which feels as though it suddenly hits your fingers and falls away just as quickly. You could try feeling at the brachial artery and raising the arm above the patient's heart. Sometimes referred to as a waterhammer pulse.
Pulsus bisferiens: a waveform with 2 peaks, found where aortic stenosis and regurgitation co-exist.
Hypertrophic cardiomyopathy: this pulse may feel normal at first but peter out quickly. Often described as jerky.
Pulsus alternans: an alternating strong and weak pulsation, synonymous with a severely impaired left ventricle in a failing heart.
Pulsus paradoxus: pulse is weaker during inspiration (causes include cardiac tamponade, status asthmaticus, and constrictive pericarditis).
Graphical representation of different arterial pulse waveforms and their causes
Friday, 31 December 2010
Cardiac Pacemaker
It is represents External Energy Sources Used To Stimulate The Heart Primarily In Patients With Symptomatic Heart Blocks And Bradyarrhythmias.
Indication :
* Selection Of The Appropriate Pacemaker And Pacing Mode Depends On The Clinical Condition And The Type Of Bradyarrhythmia Being Treated* Temporary Pacing :
- For Symptomatic Bradicardia Due To Temporary Condition, Or As A Bridge To Permanent Pacer Placement
- Symptomatic Bradycardia Due To : SA Nodal Dysfunction, Irreversible 2nd Or 3rd Degree AV Block
- Recurrent Syncope Due To Carotid Sinus Hypersensitivity
- Chronotropic Incompetence Is Present
- An Increase In Heart Rate Is Required To Enchance Physiologic Performance
Thursday, 30 December 2010
Mapping the Atrioventricular Node

A 75-year-old woman presented with dyspnea, an awareness of rapid heart action, and permanent atrial fibrillation with a rapid ventricular response that had been resistant to treatment with beta-blockers, calcium-channel blockers, digoxin, and multiple cardioversions. For severe rheumatic aortic and mitral stenosis, she had undergone replacement of the aortic and mitral valves with Starr–Edwards devices in 1970, as seen on chest radiography on admission (Panels A and B, arrows). In 2006, a pacemaker had been implanted for the treatment of bradycardia.
To control the rapid ventricular response to atrial fibrillation, the patient underwent ablation of the atrioventricular node, located just below the aortic valve, where the ablation catheter was positioned (Panel C). Whereas ablation sites are often identified with the use of computerized systems for "electroanatomical mapping," the patient's atrioventricular node was identified on the basis of simple anatomical landmarks, the aortic and mitral valves. The atrioventricular node may be injured by operations or infections because of its proximity to these valves.
After ablation, the patient's condition immediately improved. Atrioventricular-node blocking agents were discontinued, and the only cardiac medications she continued to receive were warfarin and furosemide. Six months after the procedure, the patient remained free of heart-failure symptoms.
Sunday, 26 December 2010
Myocardial ischemia in older patients
Which of the following symptoms is more likely to represent myocardial ischemia in older patients?
The answer is B.
Exertional angina (chest pain) is the most common manifestation of myocardial ischemia in young and middle-age persons. Because of their more sedentary lifestyle or possibly a difference in pathophysiology, this may not be true in elderly patients. Instead of exertional chest pain, ischemia may be more commonly manifested as dyspnea in elderly patients. Other elderly patients with CAD may be completely asymptomatic, although silent ischemia may be demonstrated by stress testing or Holter monitoring.
- A) Chest pain
- B) Dyspnea
- C) Diaphoresis
- D) Back pain
- E) Jaw pain
Answer and Discussion
The answer is B.
Exertional angina (chest pain) is the most common manifestation of myocardial ischemia in young and middle-age persons. Because of their more sedentary lifestyle or possibly a difference in pathophysiology, this may not be true in elderly patients. Instead of exertional chest pain, ischemia may be more commonly manifested as dyspnea in elderly patients. Other elderly patients with CAD may be completely asymptomatic, although silent ischemia may be demonstrated by stress testing or Holter monitoring.
Note:
Instead of exertional chest pain, ischemia may be more commonly manifested as dyspnea in elderly patients.
Monday, 20 December 2010
A case of Giant Left Atrium

An 83-year-old woman with long-standing atrial fibrillation who had previously undergone atrioventricular nodal ablation and pacemaker placement presented with symptoms of progressive heart failure.
Physical examination was notable for elevated jugular venous pressure, precordial lift, a grade 2/6 holosystolic murmur at the sternal border and apex, hepatomegaly, ascites, and severe lower-extremity edema.
Laboratory evaluation revealed a creatinine level of 1.4 mg per deciliter (124 µmol per liter), an albumin level of 3.6 g per deciliter, and a brain natriuretic peptide level of 526 pg per milliliter (normal range, 0 to 100 pg per milliliter); liver function was normal.
Chest radiography
An echocardiogram
An esophagogram
The patient was discharged home on medical management after prolonged diuresis.
Thursday, 16 December 2010
Shapes of Arterial pressure waves
While palpating the pulse of a patient, you note that the pulse wave has two peaks. You auscultate the heart and are certain that there is only one heartbeat for each two
pulse waves. Which of the following best describes this finding?
. The answer is: ( e ).
Pulsus bisferiens (bisferious pulse) is seen in AI and in hypertrophic cardiomyopathy (HCM). In the latter, the first wave or percussion wave is due to the rapid flow rate of initial contraction, and the second wave or tidal wave is due to the slower rate of continued contraction. The dicrotic pulse has two palpable pulses, but one is in systole and the other is in diastole.
Pulsus bigeminus is an alteration in pulse amplitude that follows a ventricular premature beat. Pulsus alternans is a regular alternating pulse amplitude due to alternating left ventricular contractile force; it is usually seen with severe left ventricular decompensation and cardiac tamponade. Pulsus parvus et tardus(“small and slow rising”) represents a delayed systolic peak due to obstruction to left ventricular ejection. It is seen in aortic stenosis (AS)
pulse waves. Which of the following best describes this finding?
- a.Pulsus alternans
- b.Dicrotic pulse
- c.Pulsus parvus et tardus
- d.Pulsus bigeminus
- e.Pulsus bisferiens
. The answer is: ( e ).
Pulsus bisferiens (bisferious pulse) is seen in AI and in hypertrophic cardiomyopathy (HCM). In the latter, the first wave or percussion wave is due to the rapid flow rate of initial contraction, and the second wave or tidal wave is due to the slower rate of continued contraction. The dicrotic pulse has two palpable pulses, but one is in systole and the other is in diastole.
Pulsus bigeminus is an alteration in pulse amplitude that follows a ventricular premature beat. Pulsus alternans is a regular alternating pulse amplitude due to alternating left ventricular contractile force; it is usually seen with severe left ventricular decompensation and cardiac tamponade. Pulsus parvus et tardus(“small and slow rising”) represents a delayed systolic peak due to obstruction to left ventricular ejection. It is seen in aortic stenosis (AS)
CLICK FOR MORE DETAILES
Sunday, 12 December 2010
Friday, 10 December 2010
Compensatory mechanisms that 'save' organ blood flow
Effects of inadequate perfusion on cell function.
Heart compensatory mechanisms that 'save' organ blood flow during shock is collected in "Heart SAVER":
- Symphatoadrenal system activation
- Atrial natriuretic factor release
- Vasopressin release
- Endogenous digitalis-like factor release
- Renin-angiotensin-aldosterone system activation
Wednesday, 8 December 2010
Rheumatoid nodules appearance

These are a focus of central fibrinoid necrosis surrounded by a palisade of epitheloid cells, occurring as a typical feature of sero-positive rheumatoid arthritis.
Subcutaneous nodules commonly occur on extensor surfaces subject to external pressure, for example, the upper forearm and elbow. Occasionally, they arise within the lungs or heart.
Nodules are rare in sero-negative rheumatoid arthritis.
Friday, 3 December 2010
A case of Digoxin toxicity
A 96-year-old African American female was admitted from a nursing home with complaints of abdominal pain, nausea and vomiting (N/V), dizziness, confusion and double vision for 5 days. She was discharged from the hospital just 4 days ago. Digoxin was started during that previous hospitalization for control of tachycardia in atrial fibrillation. One day prior to discharge, digoxin level was 1.8 mg/mL and digoxin dose was decreased to 125 mcg PO Q 48 hr.
Past history of Hypertension, atrial fibrillation, coronary artery disease, stroke, congestive heart failure.
Medications
Metoprolol, digoxin, ASA (aspirin), lisinopril, furosemide (Lasix), Coumadin (warfarin), esomeprazole (Nexium).
On Physical examination
In pain, combative and confused.
VSS.
Chest: Occasional bibasilar crackles.
Cardiovascular System: Clear S1 and S2, irregularly irregular rhythm, HR 101 bpm.
Abdomen: Soft, epigastric tenderness, no rebound, + BS.
Extremities: No edema.
the most likely diagnosis :
Digoxin toxicity.

Laboratory results:
This Figure shows Digoxin toxicity. Treatment with digoxin was started in the hospital and the patient was discharged to SNF, she was re-admitted 4 days later with digoxin toxicity.
What would you do?
Stop digoxin.
Monitor digoxin levels.
Control symptoms.
Sitter in the room.
Summary
Digoxin toxicity was first described in 1785.
Approximately 0.4% of all hospital admissions, 1.1% of outpatients on digoxin, and 10-18% of nursing home patients develop toxicity. Advanced age ( older than 80 years) is an independent risk factor associated with increased morbidity and mortality.
Serum concentrations associated with toxicity overlap between therapeutic and toxic ranges because of the many factors which can potentiate digoxin toxicity.
Past history of Hypertension, atrial fibrillation, coronary artery disease, stroke, congestive heart failure.
Medications
Metoprolol, digoxin, ASA (aspirin), lisinopril, furosemide (Lasix), Coumadin (warfarin), esomeprazole (Nexium).
On Physical examination
In pain, combative and confused.
VSS.
Chest: Occasional bibasilar crackles.
Cardiovascular System: Clear S1 and S2, irregularly irregular rhythm, HR 101 bpm.
Abdomen: Soft, epigastric tenderness, no rebound, + BS.
Extremities: No edema.
the most likely diagnosis :
Digoxin toxicity.

Laboratory results:
This Figure shows Digoxin toxicity. Treatment with digoxin was started in the hospital and the patient was discharged to SNF, she was re-admitted 4 days later with digoxin toxicity.
What would you do?
Stop digoxin.
Monitor digoxin levels.
Control symptoms.
Sitter in the room.
Summary
Digoxin toxicity was first described in 1785.
Approximately 0.4% of all hospital admissions, 1.1% of outpatients on digoxin, and 10-18% of nursing home patients develop toxicity. Advanced age ( older than 80 years) is an independent risk factor associated with increased morbidity and mortality.
Serum concentrations associated with toxicity overlap between therapeutic and toxic ranges because of the many factors which can potentiate digoxin toxicity.
Wednesday, 1 December 2010
Subscribe to:
Posts (Atom)